TLDR;
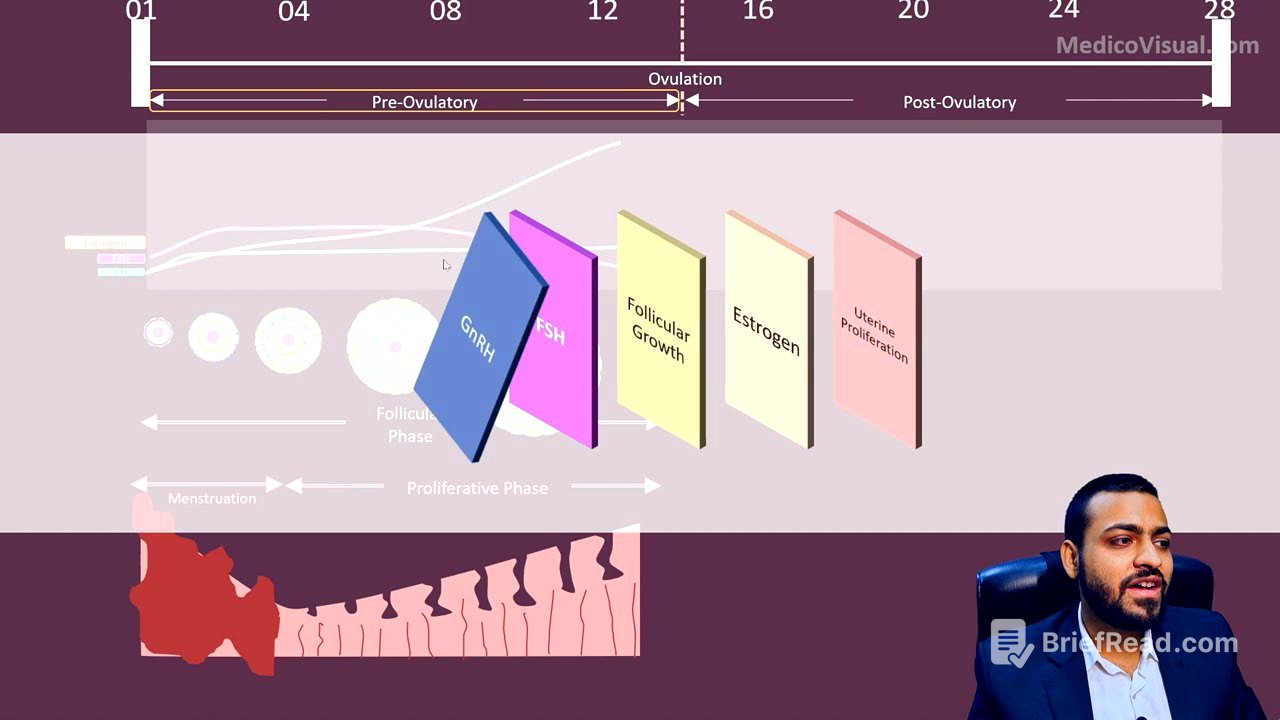
This video explains the pre-ovulatory phase of the female reproductive cycle, focusing on the events leading up to ovulation. It covers the development of follicles, the roles of FSH and LH, the formation of the theca and granulosa cells, the influence of estrogen on the uterus, and cervical changes.
- Primordial follicles develop into primary follicles under the influence of FSH and LH.
- Theca cells produce testosterone, which granulosa cells convert to estrogen.
- Estrogen stimulates the proliferation of the endometrium in the uterus.
- Cervical changes, including increased elasticity and thin, watery mucus, facilitate sperm entry.
Intro [0:00]
The lecture will discuss the pre-ovulatory phase of the female reproductive cycle, detailing the events that occur before ovulation.
Menarche and Menopause [1:53]
Menarche is the start of the menstrual cycle in a female's life, typically around 13 or 14 years old. The menstrual cycle continues monthly until menopause, which occurs around the age of 50.
Folliculogenesis [3:07]
Each month, 15 to 20 primordial follicles start growing, but only one becomes the dominant follicle and is released into the fallopian tube. The flattened follicular cells of a primordial follicle grow into cuboidal cells, transforming it into a primary follicle. A zona pellucida, a glycoprotein layer with species-specific sperm receptors, forms between the follicular cells and the oocyte.
Role of Hypothalamus and Anterior Pituitary (Gonadrophs) in releasing FSH and LH [6:06]
The hypothalamus releases gonadotrophin-releasing hormone (GnRH), which stimulates the anterior pituitary to release gonadotrophs, specifically FSH and LH. These hormones nourish and help the follicles grow inside the ovary. The follicular phase is variable and affected by a woman's mood and environmental factors because it is controlled by the hypothalamus.
Levels of FSH and LH (Gonadotrophins) rises in blood during follicular phase [9:38]
FSH and LH levels rise in the blood, affecting the follicles in the ovaries. The development from primordial to unilaminar primary follicle is independent of FSH and LH. Beyond this point, FSH is crucial for follicle growth. FSH stimulates the primary follicle to proliferate, increasing both the size and number of follicular cells, and the size of the primary oocyte. The primary follicle becomes multilaminar.
Theca formation and it's importance [12:15]
Interstitial connective tissue surrounds the follicle, forming a theca, which consists of two layers: theca interna (more cellular) and theca externa (more vascular). LH acts on theca interna cells, causing them to release testosterone. Follicular cells convert this testosterone into estrogen using the enzyme aromatase.
Estrogen level begin to rise as follicules grow [17:30]
As follicles grow, estrogen levels rise in the blood. Follicular cells become filled with granules of estrogen and are now called granulosa cells. Estrogen induces the formation of LH receptors on granulosa cells.
Estrogen causes Proliferation of endometrium of uterus [18:04]
Estrogen orders the uterus to prepare for a potential pregnancy by causing the endometrium to proliferate. The endometrium forms multiple layers: the basal layer (stratum basalis), the spongy layer (stratum spongiosum), and the compact layer (stratum compactum).
Formation of Follicular fluid (antrum) [21:24]
Pockets of follicular fluid form between the follicular cells and coalesce to form an antrum. At this stage, the follicle is now a secondary follicle, though the oocyte within remains a primary oocyte arrested in prophase one of meiosis one.
All non-dominant follicles undergo Follicular Atresia (death) [25:13]
Of the 15 to 20 primordial follicles that begin to grow, only one becomes the dominant follicle. As estrogen levels rise, FSH levels decline. The dominant follicle, now independent of FSH, survives, while the non-dominant follicles, still dependent on FSH, undergo follicular atresia (death).
Dr. Najeeb's Analogy (Mnemonic) [28:16]
Dr. Najeeb's analogy illustrates this concept: the anterior pituitary is like a father providing financial support (FSH) to growing follicles (children). As the follicles produce their own estrogen (cash), the pituitary reduces its support (FSH). Only the dominant follicle, financially independent, survives.
Review [29:55]
The pre-ovulatory phase, also known as the follicular phase of the ovarian cycle, involves follicular growth and estrogen production. In the uterus, the functional uterine wall (stratum spongiosum and stratum compactum) is shed during menstruation in the first five days, followed by the proliferation of the endometrium under the influence of estrogen.
Cervical changes in the pre-ovulatory phase of female menstrual cycle [32:37]
The cervix, the lower part of the uterus connecting it to the vagina, undergoes changes during the pre-ovulatory phase. The cervical os slightly opens up, and the cervix becomes elastic and soft due to high estrogen levels. Cervical glands secrete hair-like strands of mucus arranged parallel to each other to welcome sperm. The cervical mucus becomes thin and watery, facilitating sperm movement.
High levels Estrogen increase Libido in females [36:42]
As estrogen levels peak, there is a slight dip in basal body temperature. High estrogen levels also cause an increase in libido in females during this fertile period.